The Recipe to a Healthy Heart:Your Guide to Preventing Heart Disease
Sure, the taste of food is important, but do you know how your diet impacts your heart? Many foods contain hidden ingredients that negatively impact...

Cleerly’s Medical Affairs team had the opportunity to present at the American Heart Association’s (AHA) 2022 Scientific Sessions this past week in Chicago. This event brings together the brightest scientific and clinical minds in cardiovascular and brain health science to discuss the latest discoveries and innovations coming out of our fields.
At AHA, our Founder and CEO, James Min, MD, presented in a session titled, “Advanced Cardiac Imaging: Risk Profiling and Precision Heart Health Driven by AI-Enabled CV Imaging” in the Health Innovation Pavilion‚ Heart Hub‚ Science and Technology Hall‚ Le. In the presentation, he discussed our preventive approach to cardiac care, why this approach is critical to the transformation of med tech and how preventive measures are driving technological trends.

"We’d like to try to usher the field of cardiology away from population-based estimates into precision heart care to pinpoint an individual who’s at risk, and then to translate and educate these people in a way that you can just look at a screen and know who’s sick and who’s not."
Additionally, we showcased a number of abstracts, highlighting the research underway that demonstrates how Cleerly accurately identifies lipid-rich plaque and defines the optimal definition of high-risk plaque by computed tomography angiography (CTA). Through our research, we also identified a novel metric to better define high-risk plaques with coronary CT angiography (CCTA).
.png?width=450&height=203&name=image%20(10).png)
In this study, we looked at if artificial intelligence-enabled quantitative CT (AI-QCT) would enable identification of the optimal Hounsfield threshold (HU) for lipid-rich plaques when compared to invasive near-infrared spectroscopy intravascular ultrasound (NIRS-IVUS) reference standard. Our team studied atherosclerotic plaques from patients using three different low-density non-calcified plaque (LD-NCP) thresholds (30,50, and 70 HU) and analyzed by sensitivity, specificity, positive and negative predictive value, accuracy, and area under the curve (AUC). We found that use of a <30 HU threshold for defining LD-NCP on AI-QCT correlates optimally with the necrotic core depicted with NIRS-IVUS (maxLCBI4mm ≥ 400).
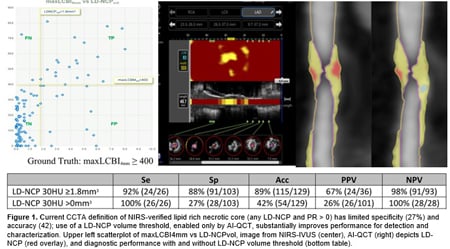
In this study, we examined what the optimal AI-QCT criteria would be to identify lipid-rich plaques when compared to the NIRS-IVUS as a reference standard. We also compared vessel area, plaque burden, minimal lumen area and plaque length between intravascular ultrasound (IVUS) and AI-QCT. The results showed that a minimum threshold of 2.3 mm3 of LD-NCP on AI-QCT has excellent correlation with NIRS-IVUS in identifying lipid-rich plaques and substantially increases accuracy and specificity compared with the current clinical definition.
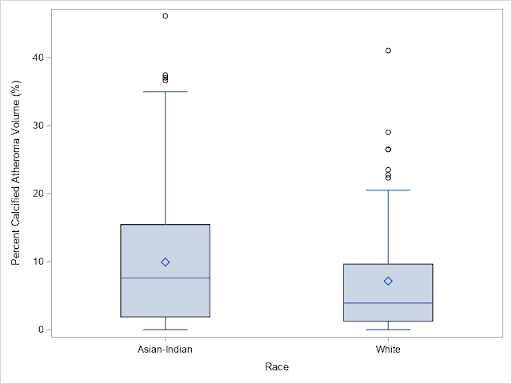
South Asians (SA) have greater atherosclerotic cardiovascular disease (ASCVD) rates than Non-Hispanic Whites (NHW) and SA ethnicity is a risk factor for cardiovascular disease, according to American College of Cardiology (ACC) and AHA guidelines. However, data on the phenotypic expression of atherosclerosis in SA is limited. This study examined plaque burden in SA using quantitative plaque analysis from CCTA. This cross-sectional study compared the prevalence of atherosclerosis in 104 SA to that of 104 propensity matched NHW.
SA had significantly higher calcified plaque percent atheroma volume PAV and higher prevalence of obstructive disease compared to the NHW cohort, which may explain the greater incidence of cardiovascular events and supports the guidelines mentioned above.
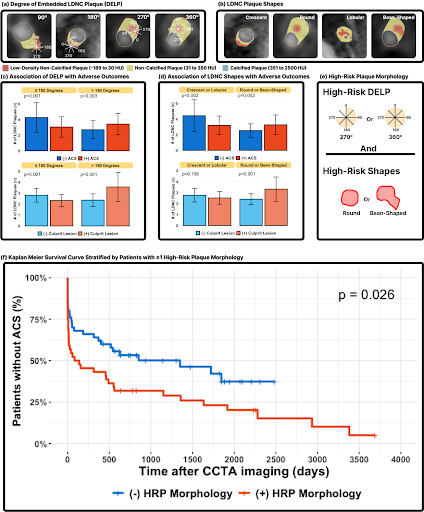
We defined a new definition for high risk plaque which we call HRP morphology. This states that the shape of the low-density non-calcified coronary plaque must be round or bean shaped and must be surrounded by non-calcified plaque for at least 270 degrees circumferentially. Using this new definition we tested to see if it was associated with acute coronary syndrome (ACS) and culprit lesion precursors from the ICONIC Study. Our conclusion was that the newly defined high-risk plaque (HRP) morphology may substantially improve the stratification of patients at risk for ACS.
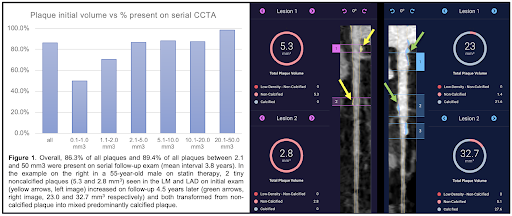
Non-obstructing small coronary plaques are not always identified during routine clinical reads of CCTA but may be identified by AI-QCT. However, it’s unclear if these are true early atherosclerotic plaques or false positive findings. We examined if serial CCTA exams can provide insights into the natural history of these findings, as a plaque appearing in the same anatomical location and demonstrating interval change is likely real. 399 plaques measuring between 0.1 and 50.0 mm3 were identified using AI-QCT in 83 patients with serial CCTA exams (N=166 exams) from our PARADIGM Trial.. Serial studies were processed in a blinded manner and linked after processing. The presence and change in plaque characteristics were assessed. Small coronary plaques depicted with serial AI-QCT are often present in the same location upon follow-up, increase in volume and develop or increase calcification with statin therapy. While further data regarding the natural history and prognosis of these plaques is warranted, our findings provide a rationale for identifying early coronary atherosclerotic plaques.
As we continue our work to change the current standard of cardiovascular care, these conferences have a great impact. The research presented is critical to the future of heart disease prevention. Our Medical Affairs team was grateful for the opportunity to network with global thought leaders on basic, clinical and population science that is poised to drastically improve how we identify heart disease and the cardiology field. We thank the American Heart Association for putting time and effort into the Scientific Sessions each year!
Want to learn more about Cleerly?
CONNECT WITH US

Sure, the taste of food is important, but do you know how your diet impacts your heart? Many foods contain hidden ingredients that negatively impact...

As we reach the end of 2023 and yet another remarkable year at Cleerly, it’s a great opportunity to reflect on all we’ve accomplished and begin...

Cleerly has had a busy few months – attending conferences, panel sessions, and winning awards as we all work together to achieve our mission of a...

1 min read
Findings from Cleerly's groundbreaking echo the recent American College of Cardiology guidelines on the use of CCTA for non-invasive heart disease...

1 min read
Cleerly CEO James Min, M.D., is a guest on the latest episode of the AWS Health Innovation Podcast hosted by Joe Shonkwiler, M.D.

1 min read
Cleerly Episode Featured on the AHA's Advancing Health Podcast Series Dr. Leon D. Caldwell, Senior Director, Health Equity Strategies and Innovation,...