The Recipe to a Healthy Heart:Your Guide to Preventing Heart Disease
Sure, the taste of food is important, but do you know how your diet impacts your heart? Many foods contain hidden ingredients that negatively impact...
4 min read
 Cleerly
:
February 27, 2023
Cleerly
:
February 27, 2023
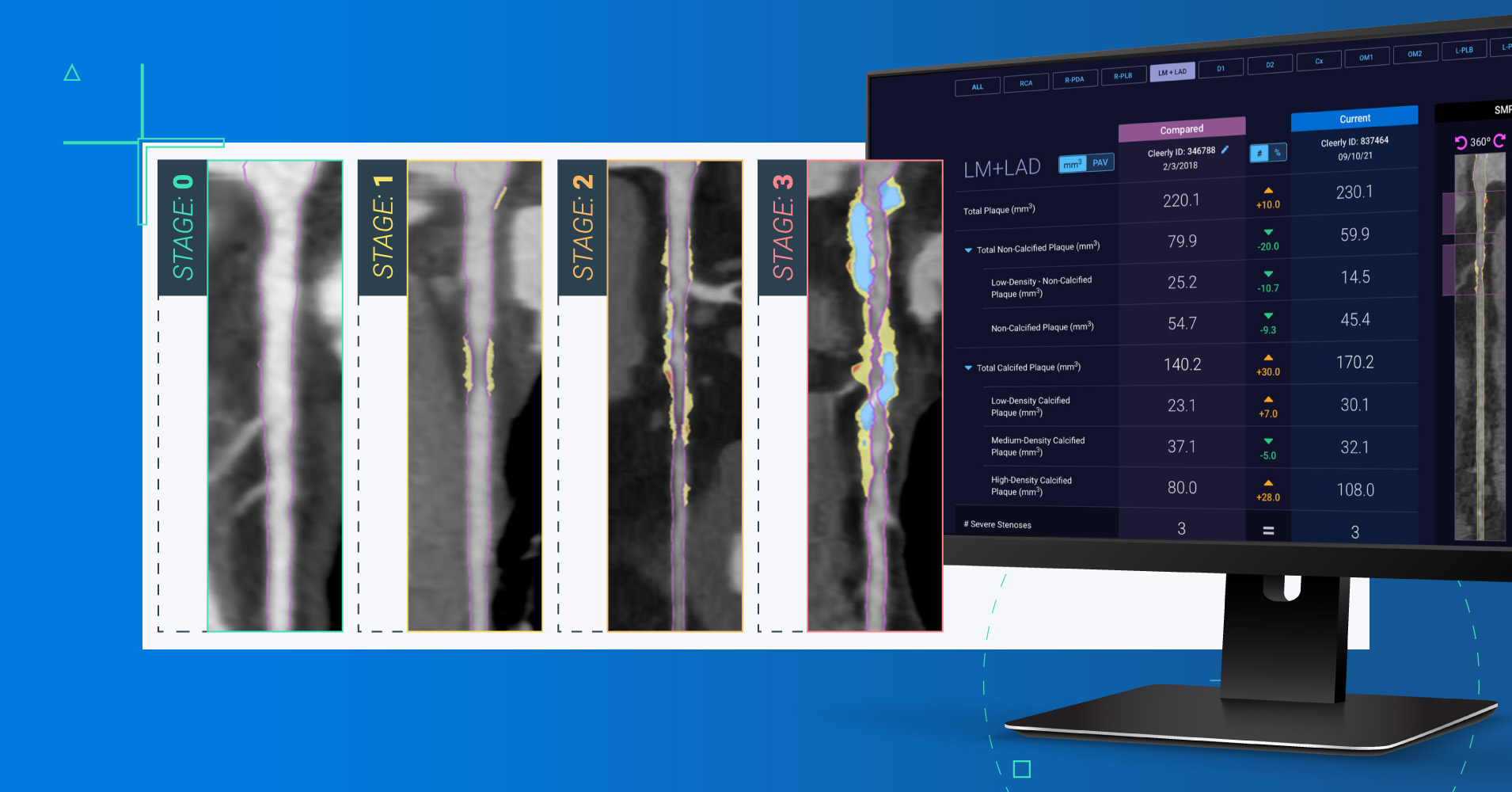
Quantification of coronary artery disease (CAD) burden and atherosclerotic plaque type has been shown to be the strongest determinant of future risk of major adverse cardiac events (MACE).1 Until recently, though, there had been no clinically useful thresholds to help physicians understand a patient’s plaque burden in its entirety to guide CAD diagnosis and management.
Instead, treatment decisions have been all too often based on indirect markers of atherosclerosis. This can result in poor outcomes – 70% of patients who suffer a heart attack had been considered low risk due to the absence of secondary symptoms,2 while nearly two-thirds of referrals for invasive evaluations of the heart based on the presence of secondary symptoms are in fact unnecessary.3
In a recent expert consensus paper in The American Journal of Medicine,4 the Innovations in Prevention Working Group of the American College of Cardiology has introduced the Atherosclerosis Treatment Algorithms. These algorithms provide personalized recommendations for medical interventions based on the combination of coronary computed tomography angiography (CCTA) quantification of atherosclerotic plaque burden and traditional cardiovascular risk factors from existing clinical guidelines.
The Atherosclerosis Treatment Algorithms use an atherosclerosis staging system for classifying disease by disease burden, published for the first time earlier this year. To the best of our knowledge, it is the first treatment pathway for heart attack prevention that directly links plaque severity and progression to personalized recommendations for therapy selection and therapy changes, respectively.
| Stage of Atherosclerosis | Angiographic Stenosis Severity | Total Plaque Volume (mm3 ) | Percent Atheroma Volume (%) |
|---|---|---|---|
| Stage 0 | No stenosis | 0 | 0% |
| Stage 1 | 1-49% stenosis 1-Vessel CAD >50% stenosis |
>0 to 250 | >0%-5.0% |
| Stage 2 | 2-Vessel CAD >50% stenosis | 250-750 | >5.0%-15% |
| Stage 3 | 3-Vessel CAD >50% stenosis | >750 | >15.0% |
CCTA is a non-invasive, highly-accurate method5 of measuring atherosclerotic burden with a low radiation dose.6 It enables a whole-heart quantification of plaque as opposed to a proximal view of single arteries. In addition, when scans are performed at regular intervals, CCTA can be used to assess changes to plaque composition over time.
Much like the atherosclerosis staging system, the treatment algorithms are based on similar prevention models for other common conditions, primarily cancer. In these instances, non-invasive imaging has made it possible to visualize, stage, and classify a disease. With this information, physicians have information that makes it possible to personalize treatment plans based on individual disease characteristics, assess the effectiveness of a given therapy, and change treatment plans over time.
What’s more, the treatment algorithms have been written specifically to account for comorbidities above and beyond atherosclerosis. For example, a patient with Stage 2 atherosclerosis (moderate plaque) and a diagnosis of Type 2 diabetes may receive the recommendation to be prescribed a GLP-1 receptor agonists in addition to a high intensity statin. Meanwhile, a Stage 1 patient (mild plaque) with a diagnosis of dyslipidemia may receive a recommendation to take a statin to manage their cholesterol.
In other words, the Atherosclerosis Treatment Algorithms are positioned to support personalized care pathways for patients based on their individual disease burden, comorbidities, and clinical risk factors. This approach is poised to shift cardiovascular care from a model of reactive response to one of preventive care – and to help providers personalize treatment for millions of Americans every year.
| Stage | Treatment | Serial CCTA* |
|---|---|---|
| Stage 0 |
|
4 years |
| Stage 1 |
|
3 years |
| Stage 2 |
|
2 years |
| Stage 3 |
|
1 year |
*Perform serial coronary CT angiographies (CCTA) until plaque stabilization or plaque regression has been achieved.
It’s important to note that the treatment algorithms are not intended to serve as a replacement to practice guidelines or consensus statements, nor are they expected to be divorced from risk factor scoring. In addition, treatment algorithms must be validated through randomized trials and observational cohort studies.
That said, the authors of the paper – Cleerly CEO James Min, MD and CMO James Earls, MD, along with representatives from eight leading U.S. medical schools – indicated that the algorithms are expected to evolve to include features such as atherosclerotic plaque composition and diffuseness as well as the presence of high risk plaques.
"We anticipate that there will be a flurry of clinical research in this new field of therapy based upon personalized phenotypic coronary artery disease expression, rather than sole reliance on traditional risk factors. This is the future of cardiovascular care," Earls said.
Disclaimer: The information provided herein is for informational purposes only and does not constitute a recommendation, representation, warranty, statement, or guarantee of any kind. The atherosclerosis treatment algorithms (ATA) are not intended to serve as a replacement to practice guidelines or consensus statements, nor are they expected to be divorced from risk factor scoring. The ATAs are based on the combination of CCTA screenings and traditional cardiovascular risk factors from existing clinical guidelines and are planned to be validated through randomized trials and observational cohort studies.
References
1. Atherosclerosis. Nature Reviews Disease Primers. August 16, 2019.
2. Preventing Myocardial Infarction in the Young Adult in the First Place. Journal of the American College of Cardiology. May 2003.
3. Low Diagnostic Yield of Elective Coronary Angiography. New England Journal of Medicine. March 11, 2010.
4. Coronary Atherosclerosis Burden and Progression to Guide Clinical Decision Making: A Report from the American College of Cardiology Innovations in Prevention Working Group. The American Journal of Medicine. December 10, 2022.
5. Coronary CT angiography versus intravascular ultrasound for estimation of coronary stenosis and atherosclerotic plaque burden: a meta-analysis. Journal of Cardiovascular Computer Tomography. August 23, 2013.
6. The sub-millisievert era in CTCA: the technical basis of the new radiation dose approach. La radiologia medica. September 15, 2020.

Sure, the taste of food is important, but do you know how your diet impacts your heart? Many foods contain hidden ingredients that negatively impact...

As we reach the end of 2023 and yet another remarkable year at Cleerly, it’s a great opportunity to reflect on all we’ve accomplished and begin...

Cleerly has had a busy few months – attending conferences, panel sessions, and winning awards as we all work together to achieve our mission of a...

1 min read
Cleerly attended the American College of Cardiology conference (ACC.23/WCC) to showcase our efforts in providing a safe and effective approach to...

1 min read
When patients present to physicians with an elevated risk of coronary artery disease, or CAD, cardiologists have many tests at their disposal....

1 min read
"It's very scary because I had a lot of patients and even friends and neighbors that had heart attacks, and we thought they were healthy by eating...